Request a consultation about proton therapy cancer treatment
To learn more about proton therapy or to schedule a consult, please fill out the form below and someone will contact you to answer your questions.
What is Proton Therapy for Lung Cancer?
Powerful Treatment With Pinpoint Accuracy
With the utmost precision, our expert physicians target lung cancer with powerful protons while sparing nearby healthy tissues and organs from unwanted radiation.
As one of the most advanced forms of radiation therapy available, proton therapy dramatically reduces radiation exposure to surrounding vital organs and lowers the occurrence of side effects. Where standard X-ray radiation can irradiate the heart, esophagus, and spinal cord in the process of radiating the tumor, proton therapy deposits radiation directly into the tumor without exiting through healthy tissue.
Treating Lung Cancer with Proton Therapy in New Jersey
Conventional X-ray radiation and proton therapy both destroy cancer cells by preventing them from dividing and growing. But it is the unique properties of protons – positively charged atomic articles – that allow our radiation oncologists to selectively target tumors of the lung and limit excess radiation exposure.
With proton therapy, a higher radiation dosage can be controlled and deposited directly into the tumor site while protecting surrounding healthy tissue. This precision is particularly important for lung cancer given the tumor’s close proximity to critical and sensitive structures, such as the esophagus, heart, spinal cord, and healthy lung.
The precise quality of proton therapy means treatment is less invasive with a lower risk of side effects, such as pneumonitis and esophagitis, and lower odds of secondary cancers. With less side effects both during and after treatment, patients can continue to enjoy their usual activities with little interruption.
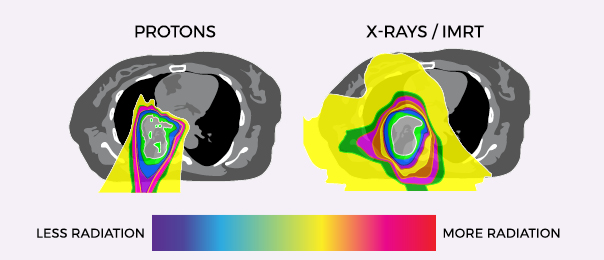
Proton Therapy vs X-Ray/IMRT for Lung Cancer
Proton Therapy delivers less radiation to the lungs and other nearby organs than X-ray radiation. These images show the areas of the body exposed to radiation during treatment. Where standard X-ray radiation releases radiation from the moment it penetrates the skin and all the way through to the other side of the tumor, proton therapy deposits radiation directly into the tumor without exiting through surrounding healthy tissue.
Benefits of Proton Therapy for Lung Cancer
- Ultra-precise treatment delivers radiation directly into the tumor, maximizing the dose to lung cancer cells
- No exit dose minimizes radiation exposure to nearby healthy tissues and critical organs, including the heart, spinal cord, esophagus, and healthy lung
- More radiation directly to the tumor improves outcomes for lung cancer patients1
- As effective as conventional X-ray radiation (3D-CRT and IMRT) with lower side effects such as pneumonitis (inflammation of the lung), pericarditis (inflammation of the heart) and esophagitis (inflammation of the esophagus)
- Can be used as a follow-up to surgery or chemotherapy
- Minimally invasive treatments allow patients to maintain their quality of life both during and after treatment
- FDA-approved treatment

Studies show that proton therapy is as effective as X-ray radiation in treating non-small cell lung cancer (NSCLC) and can reduce side effects such as pneumonitis, pericarditis, and esophagitis (inflammations of the lungs, heart, and esophagus).2
Is Proton Therapy for Lung Cancer Right for Me?
Many patients with stage I, II or III non-small cell lung cancer (NSCLC) and certain stages of small cell lung cancer (SCLC) are good candidates for proton therapy.
Proton therapy may be an especially good treatment option for you if:
- your tumor is near critical structures such as the spine, heart and esophagus
- you need concurrent chemotherapy with reduced radiation to bone marrow
- have had prior radiation therapy
- have limited or poor pulmonary function due to COPD, prior smoking history, or other medical conditions.
If you are interested in proton therapy as a treatment option, ProCure can schedule a consultation with one of our radiation oncologists to determine if you are likely to benefit from proton therapy. Please call us for more information.
Lung Cancer Treatment FAQs
Proton therapy is an advanced form of radiation that destroys cancer cells by preventing them from dividing and growing. Proton therapy uses protons—positively charged atomic particles—instead of the photons used in standard X-ray radiation therapy. With proton therapy, doctors can precisely target the tumor while minimizing damage to the surrounding healthy tissue. Unlike standard X-ray radiation, protons deposit much of their radiation directly in the tumor and then stop.
Treatments are usually given five days a week for one to seven weeks, depending on the stage of your cancer and other health factors.
Yes. Proton therapy can be used as a follow-up to surgery or chemotherapy.
Most patients do not feel pain or discomfort during treatment. The majority of the time patients spend in the treatment room involves setting up for treatment.
Your radiation therapists will have everything ready for you before the treatment begins. You will be moved into position before each treatment using an FDA-approved robotic positioning system. You will be asked to lie still on a treatment bed while your therapists make adjustments. After you are in position, the proton beam is delivered and is on for about one minute. You will not feel or see the proton beam. You may hear some clicking from the equipment around you, but generally, after a few treatment sessions, the sounds go unnoticed. During the actual treatment, your therapists will leave the room and monitor your treatment from a control room just outside the treatment room. Although they are not in the same room as you, they can see and hear you through a video monitor. They remain close by and you can easily talk to them if you need anything.
There is no need to stay overnight in a hospital or remain at the Center after your treatment. In most cases, you can go about your normal routine before and after your session.
ProCure treats stage I, II, and III Non-Small Cell Lung Cancer (NSCLC) and certain stages of Small Cell Lung Cancer (SCLC).
Proton therapy is covered by Medicare and many private insurance providers. ProCure has financial counselors who are dedicated to guiding you through the insurance process. Please contact us if you have questions about coverage.
Proton therapy and X-ray radiation therapy both treat lung cancer by killing cancer cells when they attempt to divide and multiply. However, there is an important difference. X-ray radiation releases its maximum dose of radiation quickly after penetrating the skin and continues to release radiation as it passes through your body beyond the tumor, exposing more tissue to unwanted radiation and potentially causing more damage to healthy tissue and organs. Proton therapy delivers most of the radiation exactly at the tumor site and then stops. There is essentially no radiation exposure beyond the tumor site once the radiation has reached and covered the treatment area. This allows proton radiation to target the tumor while reducing damage to surrounding healthy tissue.
For lung cancer, this means that proton therapy can deliver the same dose to the tumor with less radiation damage to the healthy lung tissue compared with standard radiation treatments, such as three-dimensional conformal radiation therapy (3D-CRT) and IMRT.3 Additionally, proton therapy can be used to deliver more radiation to the tumor to improve the outcomes for lung cancer patients.4 This is important because precision targeting reduces radiation to the healthy lung tissues and esophagus, which significantly lowers the rates of pneumonitis and esophagitis compared to 3D-CRT or IMRT.5
Recent studies suggest that proton therapy is just as effective as other forms of radiation, such as 3D-CRT and IMRT, in patients with NSCLC, but has lower risk of side effects such as pneumonitis and esophagitis (inflammation of the lungs and esophagus).4,5 Protons can also reduce the radiation dose to the heart. Proton therapy targets the lung tumor more precisely than other forms of radiotherapy, reducing excess radiation to the uninvolved lung, heart, and other mediastinal structures.6 In a study by the University of Texas MD Anderson Cancer Center of patients with inoperable NSCLC, proton therapy reduced dose to normal lungs, esophagus, spinal cord, and heart by a significant amount compared with other forms of radiotherapy.7,8
The most common side effects from any type of radiation treatment for lung cancer patients are esophagitis and pneumonitis. The severity of these side effects is directly related to radiation dose delivered to the lungs and esophagus. With less radiation delivered to normal tissues than standard radiotherapy options such as 3D-CRT and IMRT, proton therapy is associated with lower rates of lung and esophageal side effects.4
Many patients with stage II or stage III NSCLC and certain stages of SCLC are good candidates for proton therapy. In addition, select patients with stage I or recurrent NSCLC may be candidates for proton therapy. If you are interested in proton therapy as a treatment option, we can schedule a consultation for you to speak with one of our radiation oncologists. During the consultation, the radiation oncologist will discuss different treatment options with you and determine if you may benefit from proton therapy. The radiation oncologists at ProCure use various forms of radiation to treat lung cancer in addition to proton therapy, so they will provide you a treatment recommendation that is best for you.
Currently, there is one clinical trial for lung cancer underway at ProCure:
- A phase I/II study that compares the effects on subjects and their cancer using standard chemotherapy in combination with hypofractionated proton radiation therapy for stage II-III Non-Small Cell Lung Cancer (NSCLC). Hypofractionation is a technique that delivers higher daily doses of radiation over a shorter period of time.
For more information, please see Clinical Trials or contact the center.
LUNG CANCER FACTS
Lung cancer is the leading cause of death by cancer. More people die of lung cancer in a year than from colon, breast and prostate cancers combined.
There are three types of lung cancer: Small cell lung cancer (SCLC), non-small cell lung cancer (NSCLC) and lung carcinoid tumor.
NSCLC is by far the most common type of lung cancer, accounting for approximately 85% percent of all cases.
There are three main types of NSCLC9:
- Adenocarcinoma. Usually found in the outer part of the lung, it accounts for about 40% of all lung cancers. It occurs mostly in people with a history of smoking, but it is also the most common type of lung cancer in non-smokers.
- Squamous cell (epidermoid) carcinoma. Also linked to smoking, this type comprises 25 to 30% of all lung cancers and tends to be found in the center part of the lungs.
- Large cell (undifferentiated) carcinoma. Accounting for 10-15% of all lung cancers, it can be found in any area of the lungs.
Most lung cancers do not cause symptoms in the early stage. Therefore, the majority of lung cancer patients are diagnosed with locally advanced or metastatic disease. However, some people with early-stage lung cancer do experience symptoms, the most common being10:
- A cough that does not go away or gets worse
- Chest pain that worsens with deep breathing, coughing, or laughing
- Hoarseness
- Weight loss and loss of appetite
- Coughing up blood or rust-colored sputum (spit or phlegm)
- Shortness of breath
- Feeling tired or weak
- Lung infections such as bronchitis or pneumonia that become chronic or recurring
- New onset of wheezing
Many of these symptoms are more likely to be caused by conditions other than lung cancer, but it’s important to see your doctor right away so the cause can be found and treated if needed. If you go to your doctor when you first notice symptoms and are diagnosed with cancer, it might be at an earlier stage, when treatment is more likely to be effective.
The following have been identified as factors that increase a person’s risk for developing lung cancer11:
- Smoking. Approximately 80% of lung cancer deaths are thought to result from smoking. The longer you smoke and the more you smoke, the greater your risk.
- Secondhand smoke. Inhaling the smoke produced by others can increase your risk of developing lung cancer.
- Radon exposure. Breathing this naturally occurring radioactive gas that results from the breakdown of uranium in soil and rocks is the second leading cause of lung cancer in this country and is the leading cause among non-smokers.
- Asbestos. Exposure to asbestos increases the risk of lung cancer. Those who work with the substance are many more times likely to die of lung cancer.
- Air pollution. It is estimated that 5% of all lung cancer deaths are linked to air pollution.
Radiation therapy. People who have had radiation therapy to the chest for other cancers are at higher risk for developing lung cancer. - Personal or family history of lung cancer. People who have had lung cancer themselves or who have a family member who has had lung cancer are at a higher risk.
As lung cancers do not cause any symptoms in the early stage, there are benefits in screening high-risk patients to find tumors when they are small, when they are the most curable and before they have the chance to spread.
A type of CT scan known as low-dose CT (LDCT, sometimes called low-dose spiral or helical CT) is usually used to screen for lung cancer. This test provides more detailed pictures than chest X-rays and is better at finding small abnormalities in the lungs.
A drawback of this test, however, is that it can identify many abnormalities that require further testing but aren’t in fact cancerous. LDCT’s also expose people to a small amount of radiation with each test.
Screening
The American Cancer Society currently recommends yearly lung cancer screening with LDCT scans for high-risk patients12. Patients who meet all of the following criteria may be candidates for lung cancer screening:
- 55 to 74 years old
- In fairly good health
- Are either still smoking or have quit smoking within the last 15 years
- Have at least a 30 pack per year smoking history
High-risk patients should speak with their doctor about the benefits, limitations, and potential harms of lung cancer screening. Screening should only be done at facilities that have the right type of CT scan and that are suitably experienced in LDCT scans for lung cancer screening. The facility should also have a team of specialists that can provide the appropriate care and follow-up of patients with abnormal results on the scans.
Lung Cancer Imaging Tests
Imaging tests may be done for a number of reasons both before and after a diagnosis of lung cancer, including to:
- Help find a suspicious area that might be cancerous
- Learn how far cancer may have spread
- Look for possible signs of cancer coming back after treatment
Common imaging tests include:
- Chest X-ray
- Computed tomography (CT) scan
- CT-guided needle biopsy
- Magnetic resonance imaging (MRI) scan
- Positron emission tomography (PET) scan
- Bone scan
Diagnosis
The actual diagnosis is determined by analysis of lung cells that may be gathered from:
- Lung secretions (sputum or phlegm)
- Fluid around the lungs
- A small tissue sample via needle biopsy
- Bronchoscopy
These samples are examined in a pathology lab. If cancer is found, your physician will use information from these tests to determine a treatment plan.
Talk To Us
Find out if proton therapy is the right treatment for you. Contact our Care Team or request more information online.
Attend An Information Session
Learn more about proton therapy and our world-class Care Team. Contact the center to reserve your place.