Request a consultation about proton therapy cancer treatment
To learn more about proton therapy or to schedule a consult, please fill out the form below and someone will contact you to answer your questions.
What is Proton Therapy for Breast Cancer Treatment?
Precision treatment. Vital protection.
With laser-like accuracy, proton therapy precisely targets breast cancer while sparing surrounding healthy tissue and vital organs, including the heart and lungs.
One of the first to use proton therapy for patients with breast cancer, ProCure is here to help fight breast cancer with a powerful, non-invasive treatment that significantly reduces the risk of side effects.
Treating Breast Cancer with Proton Therapy in New Jersey
Proton therapy is a highly precise treatment for breast cancer that delivers radiation directly into the tumor and stops. Radiation exposure to surrounding healthy tissue and organs is minimized, and the risk of short and long-term side effects is drastically reduced.
Where standard X-ray radiation therapy releases the maximum dose of radiation as soon as it penetrates the skin and continues to release it as it passes through the body beyond the tumor, proton therapy targets only the tumor. Healthy tissue is therefore spared from unwanted radiation.
This precision is especially crucial for the breast region due to its proximity to many vital organs, including the heart and the lungs. Because breast cancer proton therapy is so precise, higher doses of radiation can be deposited into the tumor while reducing the potential for damage. This results in much less disruption to the patient, with many able to continue with their usual daily activities during treatment. It also lessens the risk of long-term side effects and recurring cancers.
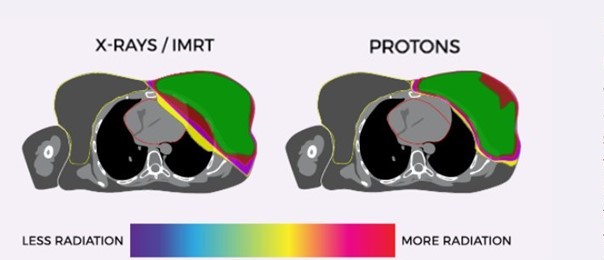
Proton Therapy vs X-Ray/IMRT for Breast Cancer
Breast cancer proton therapy spares more surrounding structures than conventional radiotherapy, including the heart, coronary arteries, lung, and contralateral breast. These images show the areas of the body exposed to radiation during treatment. Where standard X-ray treatment releases radiation from the moment it penetrates the skin and all the way through to the other side of the tumor, proton therapy deposits radiation directly into the tumor without exiting through surrounding healthy tissue. Learn more about this alternative treatment options for breast cancer when you contact us today!
Benefits of Breast Cancer Proton Therapy
- Precisely targets the tumor, maximizing the dose to breast cancer cells
- No exist dose results in lower radiation exposure to surrounding healthy tissues and critical organs
- Ultra-precision makes it highly beneficial for those diagnosed with left-sided breast cancer due to the close proximity to heart and lungs
- Lower occurrence of cardiovascular diseases compared to conventional radiation treatment
- Patients can maintain quality of life during and after treatment
- Ideal for patients who have undergone breast-conserving surgery or mastectomy
- Effective option for recurrent tumors, even in patients who have already received traditional forms of radiation
- Can be used in conjunction with surgery and chemotherapy
- Reduced odds of recurring and secondary cancers
- FDA-approved treatment
Is Proton Therapy for Breast Cancer Right for Me?
At ProCure, we treat non-metastatic breast cancers that are stages I—III.
Proton therapy may benefit you if you:
- Have non-metastatic breast cancer
- Have other risk factors that indicate a need for lymph node irradiation
- Will be receiving cardiotoxic chemotherapy
- Have pre-existing vascular comorbidity, cardiac disease or lung disease
- Have an anatomy that places normal organs at elevated risk of radiation exposure
Both patients with early stage breast cancer or locally advanced, stage III, left-sided breast cancer who have undergone either breast-conserving surgery or mastectomy may be very well treated with proton therapy.
Even if these characteristics don’t appear to fit your situation, you may still benefit from proton therapy. If you are interested in proton therapy as a treatment option, we can schedule a consultation to determine if you are likely to benefit from proton therapy. Please call us for more information.
Breast Cancer Treatment FAQs
We treat non-metastatic breast cancers that are stages I—III. We treat left- or right-sided breast cancer, after mastectomy or lumpectomy.
Similar to other forms of radiation, proton therapy is typically used in conjunction with surgery and chemotherapy and can be used to treat recurrent tumors even in patients who have already received traditional forms of radiation.
No, proton therapy does not replace the need for chemotherapy or surgery. Patients typically have proton therapy with chemotherapy or other therapies they are receiving or they receive proton therapy after surgery.
Yes. Some patients are able to have a breast implant placed before proton therapy treatment and some must wait until proton therapy is completed. Please discuss with your breast surgeon and radiation oncologist to determine the optimal timing of your reconstructive surgery and proton therapy treatment.
The time spent delivering proton therapy to the tumor is only about a minute or two, but the entire treatment session may take 30 to 60 minutes. Treatments are usually given 5 days a week for 3 to 7 weeks, depending on the stage of your cancer and other factors.
Most patients do not feel pain or discomfort during treatment. The majority of the time patients spend in the treatment room involves setting up for treatment. Your radiation therapists will have everything ready for you before the treatment begins. You will be moved into position before each treatment using an FDA-approved robotic positioning system. You will be asked to lie still on a treatment bed while your therapists make adjustments. After you are in position, the proton beam is delivered and is on for about one minute. You will not feel or see the proton beam. You may hear some clicking from the equipment around you, but generally, after a few treatment sessions, the sounds go unnoticed. During the actual treatment, your therapists will leave the room and monitor your treatment from a control room just outside the treatment room. Although they are not in the same room as you, they can see and hear you through a video monitor. They remain close by and you can easily talk to them if you need anything.
There is no need to stay overnight in a hospital or remain at the center after your treatment. In most cases, you can go about your normal routine before and after your session. Most patients have very few or mild side effects, such as fatigue, from proton therapy. If you do experience any side effects, they can be managed with medications if necessary.
Most patients with breast cancer are good candidates for proton therapy. If you would like to better understand the use of proton therapy in your treatment, we can schedule a consultation with a radiation oncologist. During the consultation, the radiation oncologist will discuss different treatment options with you and determine if you are likely to benefit from proton therapy. The radiation oncologists at ProCure use many forms of radiation to treat breast cancer, so they will provide you with a treatment recommendation for your consideration. For more information, please call us or Request More Information online.
Proton therapy is covered by Medicare and many private insurance providers. ProCure has financial counselors who are dedicated to guiding you through the insurance process. They will happily guide you and answer any questions you may have regarding insurance coverage.
We do our best to have you come to our center and speak with a physician as soon as possible, and most patients are able to schedule a consultation within one week of contacting us.
During the consultation, the radiation oncologist at ProCure will discuss different treatment options with you and determine if you can benefit from proton therapy. The radiation oncologists at ProCure use various forms of radiation to treat breast cancer in addition to proton therapy, so they will provide you with a treatment recommendation for your consideration.
Because protons deposit their energy directly into the tumor site then stop without delivering dose to the tissue behind the tumor, patients can receive lower radiation exposure to the heart, lungs, and healthy breast tissue than with X-ray radiation therapy. Less radiation to these areas will likely lower the risk of developing heart disease, lung disease, and secondary tumors decades after radiation treatment. The benefits are especially important for patients with left-sided breast cancer because the cancer is close to the heart and the lung. They are also very important for patients who have a need for radiation to lymph nodes or a coexisting heart or lung condition.
Proton therapy might be a good option if you:
- Have non-metastatic breast cancer requiring treatment to the breast/chest and regional lymph nodes
- Will be receiving cardiotoxic chemotherapy, such as doxorubicin or trastuzumab
- Have pre-existing vascular comorbidity, cardiac disease, lung disease or history of smoking
- Have anatomy that places normal organs at elevated risk of radiation exposure
Proton therapy and X-ray radiation therapy both treat breast cancer by killing cancer cells when they attempt to divide and multiply. However, there is an important difference. Because X-ray radiation releases its maximum dose of radiation quickly after penetrating the skin and continues to release radiation as it passes through your body beyond the tumor, it exposes more tissue to unwanted radiation, causing more damage to healthy tissue and organs than proton therapy.
Proton therapy delivers most of the radiation exactly at the tumor site and then stops. There is essentially no radiation exposure beyond the tumor site once the radiation has reached and covered the treatment area. With proton therapy, much less excess radiation is delivered to the heart and the lungs compared to X-ray radiation therapy.
Patients may experience mild fatigue during treatment but can continue to be active and engage in most of their normal daily activities. It is also common for patients to experience skin irritation with any type of radiation treatment for breast cancer. Your radiation oncologist can prescribe cream to help alleviate skin discomfort during your treatment.
Yes, there is clinical evidence showing that proton therapy is effective in treating breast cancer, reduces radiation dose to the heart and lung and is well tolerated by patients with low rates of side effects.
The studies showing that proton therapy is effective and well tolerated in treating breast cancer include the following:
- A study from Massachusetts General Hospital (MGH) showed that in patients with locally advanced breast cancer, post-mastectomy proton therapy was able to treat the chest wall and regional lymphatics while sparing the heart and lung from unwanted dose.1
- ProCure Proton Therapy Center and Memorial Sloan Kettering Cancer Center recently published the largest clinical study of proton therapy to treat the breast and lymph nodes. The study showed similar results as the study from MGH with patients showing very low rates of side effects. Proton therapy achieved exceedingly low exposure of radiation to the lung and heart without compromising treatment to the targeted tumor.2
The studies showing that proton therapy reduces radiation dose to the heart and lung include the following:
- A study from Paul Scherrer Institute in Switzerland compared proton therapy to standard X-ray radiation therapy for the treatment of localized breast cancer. The study shows that proton therapy covered the tumor better and lowered radiation to nearby organs when compared with standard X-ray radiation therapy. This implies that proton therapy has the potential to reduce the risk of short-term and long-term side effects.3
- A study from National Cancer Center in Korea showed that proton therapy allowed significant dose reductions to normal breast tissue, the lungs and the heart.4
- A comparative treatment planning study based on left-sided, stage III breast cancer patients treated at ProCure Proton Therapy Center showed that proton therapy significantly reduces radiation to the heart, the lung, and the breast on the opposite side of the one being treated compared to standard X-ray radiation therapies (3D-CRT, HT, and IMRT).5
A study from Swedish National Cancer (the Darby study published in the New England Journal of Medicine), a large case-control study, showed that the risk of ischemic heart disease is directly proportional to cardiac radiation dose received.6
Currently there are two trials for breast cancer underway at ProCure:
- A phase II, prospective, randomized trial comparing the effects on women with early stage breast cancer using proton radiation therapy.
- A phase II multi-institutional study conducted by the Proton Collaborative Group (PCG) to look at the rates of acute and long-term adverse events of postoperative proton radiotherapy for loco-regional irradiation in women with localized breast cancer. This study specifically includes follow-up at 10 and 15 years following proton therapy to assess the incidence of cardiac mortality and second malignant neoplasms.
For more information, please see Clinical Trials or contact the center.
Breast Cancer Facts
The most common symptom of breast cancer is a new lump or mass. A painless, hard mass that has irregular edges is more likely to be cancerous, but breast cancers can also be tender, soft or rounded.
Other potential symptoms include:7
- Swelling of all or part of a breast (even where no distinct lump is felt)
- Skin irritation or dimpling
- Breast or nipple pain
- Nipple retraction (turning inward)
- Redness, scaliness or thickening of the nipple or breast skin
- Nipple discharge (other than breast milk)
It is important to have any new breast change checked by a health care professional experienced in diagnosing breast diseases.
Average risk:8
- Gender. Being a woman is the primary risk factor. Women are 100 times more likely than men to develop the disease.
- Age. The risk of developing breast cancer increases with age. Most are found in women over 55.
- Menstrual history. Women who started menstruating before age 12 and/or went through menopause after age 55 are at a higher higher risk for developing breast cancer.
- Race and ethnicity. White women are slightly more likely to develop breast cancer than African-American women. But among women under 45 years of age, breast cancer is more common in African-American women.
- Dense breast tissue. Although not abnormal, breasts with a lot of glandular or fibrous tissue are considered dense on mammograms and such dense tissue is linked to an increased breast cancer risk.
- Having children. Women who have had no children or who had their first child after age 30 have a slightly higher breast cancer risk overall.
- Oral contraceptives. Oral contraceptive use is linked to a slightly higher risk of breast cancer.
- Hormone replacement therapy. Use of combined estrogen/progesterone hormone therapy after menopause increases the risk for breast cancer.
- Alcohol consumption. The risk of breast cancer increases with the consumption of alcohol.
- Weight. Being overweight or obese after menopause may increase breast cancer risk.
High risk:
- Genetic factors. Between 5 to 10 percent of breast cancer cases are believed to be hereditary. That means they result from gene mutations inherited from a parent. The most common is a mutation in the BRCA1 and BRCA2 genes.
- Family history. Having one first-degree relative (mother, sister, or daughter) with breast cancer nearly doubles a woman’s risk of developing the disease. Having two first-degree relatives nearly triples her risk.
- Personal history. A woman with cancer in one breast has a higher risk of developing a new cancer in the other breast or in another part of the same breast.
- Previous chest radiation. Women who, as children or young adults, had radiation therapy to the chest area have a significantly increased risk for breast cancer.
- Diethylstilbestrol (DES) exposure. Women who received, or whose mother’s received DES, have a higher risk of developing breast cancer.
- Rare disorders. Women with Li-Fraumeni syndrome, Cowden syndrome, or Bannayan-Riley-Ruvalcaba syndrome – or have a first-degree relative with one of these syndromes is at a higher risk.
Regular screening is the best way to detect breast cancer early, when the treatment needed is likely to be less aggressive and more successful.
The American Cancer Society’s current Breast Cancer Screening Guidelines recommend the following screening frequencies.9
Women with average risk:
- Between 40 and 44 should have the option to have annual breast cancer screening with mammograms.
- 55 and older should get mammograms each year.
- 55 and older can opt to have mammograms every other year, and continue screening as long as they are in good health and are expected to live at least 10 more years.
Women at high risk:
- Due to family or personal history, genetic tendency, or other risk factors should be screened with mammogram and MRI each year starting at 30.
Talk with your health care provider about your risk for breast cancer and the best screening plan for you.
Find out if proton therapy is the right treatment for you. Contact our Care Team or request more information online.
Learn more about proton therapy and our world-class Care Team. Contact the center to reserve your place.